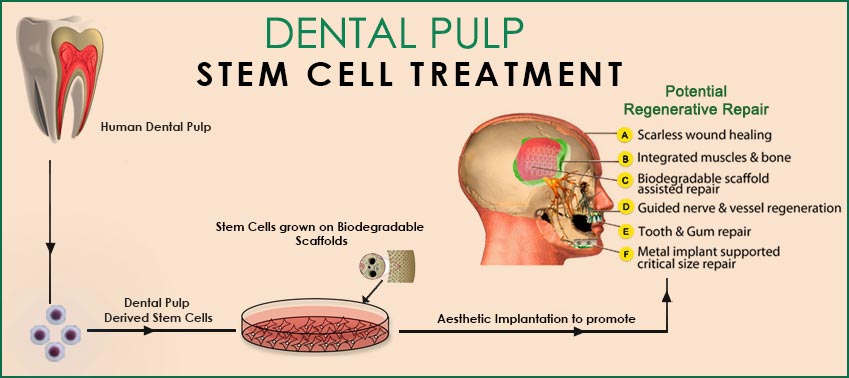
Stem cells therapy in Dentistry
training
All registered participants will receive certificates at the end of the course :
1) “Good Clinical Practice”
2) “Stem Cells therapy Expert”
Preliminary program:
Introduction
The stem cells are divided in two groups:
1) the embryonic stem cells and
2) the adult stem cells.
The latter are located in human tissues such as bone marrow, skin, adipose tissue and dental pulp
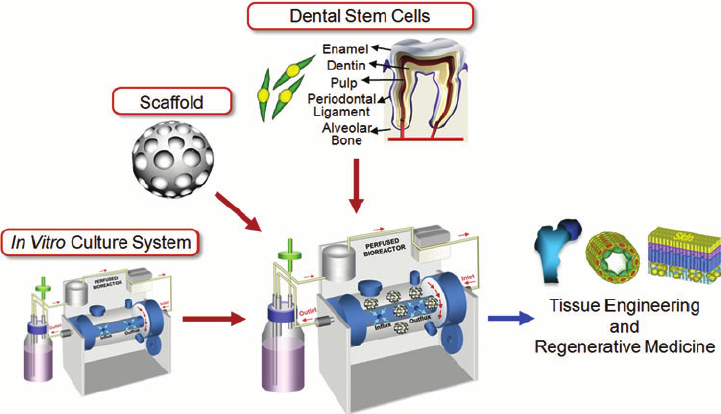
Several populations of mesenchymal stem cells are found in the tooth.
These different cell types are categorized according to their location in the tooth and they demonstrate
slightly different features. It appears that the dental stem cells isolated from the dental pulp
and the periodontal ligament are the most powerful cells for tooth engineering.
Role of epithelial stem cells, which are important for the regeneration of the enamel.
Regenerative medicine is attracting much attention because it promises new therapeutic
stem cells therapy techniques for the repair and replacement of tissues and organs that have lost functions due to ageing, disease, damage, and congenital defects .
Stem cells clinical applications have already begun to repair a wide variety of tissues, such as blood, skin, cornea, cartilage, and bone.
Dentistry has long embraced restoration of tissue and organ function.
An example of Dental Regeneration is the dental implant only recently incorporating closure with stem cell based soft tissue. Stem cells found in teeth harvested during routine dental visits are cryopreserved and appear to replicate at a higher rate than those from other parts of the body.
Stem Cells from human exfoliated deciduous teeth (SHED)
Advantages of banking SHED cells include: It’s a simple painless technique to isolate
them and being an autologous transplant they don’t possess any risk of immune reaction
or tissue rejection and hence immunosuppressive therapy is not required. SHED may also
be useful for close relatives of the donor such as grandparents, parents and siblings.
Apart from these, SHED banking is more economical when compared to cord blood and
may be complementary to cord cell banking.
The most important of all these cells are not subjected to same ethical concerns as embryonic stem cells.
Periodontal ligament stem cells (PDLSCs)
Multipotent postnatal stem cells in the human periodontal ligament (PDLSCs). When transplanted into rodents,
PDLSCs had the capacity to generate a cementum/periodontal ligament-like structure and contributed
to periodontal tissue repair. These cells can also be isolated from cryopreserved periodontal ligaments
while retaining their stem cell characteristics, including single-colony strain generation,
cementum/periodontal-ligament-like tissue regeneration, expression of MSC surface markers,
multipotential differentiation and hence providing a ready source of MSCs.
Stem cells from apical papilla (SCAP)
MSCs residing in the apical papilla of permanent teeth with immature roots are known as SCAP.
SCAP are capable of forming odontoblast-like cells,
producing dentin in vivo, and are likely cell source of primary odontoblasts for the formation of root dentin.
SCAP supports apexogenesis, which can occur in infected immature permanent teeth with periradicular periodontitis
or abscess. SCAP residing in the apical papilla survive such pulp necrosis because of their proximity to the periapical tissue vasculature.
APPLICATIONS IN DENTISTRY
Most research is directed toward regeneration of damaged dentin, pulp, resorbed root,
periodontal regeneration and repair perforations. Whole tooth regeneration to replace the traditional dental implants is also in pipeline.
Tissue-engineering applications using dental stem cells that may promote more rapid healing
of oral wounds and ulcers as well as the use of gene-transfer methods to manipulate salivary proteins and oral microbial colonization
In general,autologous bone regeneration in humans with the use of DP Stem cells in collagen sponge demonstrates optimal repair of bone defects of the mandible and the restoration of periodontal tissue
Adult dental stem cells can differentiate into many dental components, such as dentin, periodontal ligament,
cement and dental pulp tissue, but not into enamel.
The stem cells also produce a host of beneficial neurotropic factors such as glial cell lined neurotropic factor, nerve growth, and brain derived neurotropic factor, potentially promoting the survival of brain neurons lost in neuro degenerative diseases such as Parkinson’s disease.
Injecting dental stem cells into the basal ganglia can potentially provide neurotropic support for dying nerve cells and replacement of dead cells.
Intravenous injections of stem cells derived from human exfoliated deciduous tooth pulp (SHED) have a protective effect against brain damage ,stroke.
Cells extracted from dental pulp have proven to be more successfully banked and preserved than those from other sources in the body. By comparison they are more available and accessible as anticipated regenerative medical breakthroughs occur.
The use of stem cells in osseous regeneration
Adult MSCs recently identified in the gingival connective tissues (gingival mesenchymal stem cells [GMSCs]) have osteogenic potential and are capable of bone regeneration in mandibular defects.
GMSCs also suppress the inflammatory response by inhibiting lymphocyte proliferation and inflammatory cytokines and by promoting the recruitment of regulatory T-cells and anti-inflammatory cytokines.
Thus, GMSCs potentially promote the “right” environment for osseous regeneration and is currently being therapeutically explored.
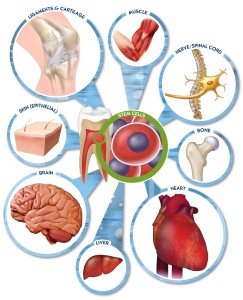
PROSPECTS OF DENTAL STEM CELLS IN MEDICINE
Dental stem cells for medical applications like heart therapies,
regenerating brain tissue, for muscular dystrophy therapies and for bone regeneration.
SHED can be used to generate cartilageas well as adipose tissue.
Bone grafting for reconstruction of large size cranial bone defects
Stem cells offer a new perspective targeting dental pulp regeneration and further development of root structure. Both SHED and DPSC can differentiate into odontoblasts
Stem cell therapies is Periodontology.
Other areas that may benefit from the development of stem cell therapies is Periodontology.
regeneration with stem cells or/and bioabsorbable matrices are the main therapies used to regenerate the periodontium tissues
Induced stem cells from harvested human dental stem cells
Our innovative method is to generate induced stem cells from harvested human dental stem cells.
Shinya Yamanaka has been recently awarded The Nobel Prize in Physiology or Medicine 2012 for generating iPSC
This approach reprograms dental stem cells into an embryonic state, thus expanding their potential to differentiate into a much wider range of tissue types.
Our stem cells lab succeeded in making specific dental tissues or tooth like structures
for regeneration of functional tooth in humans.
Banking stem cells
Obtaining and banking stem cells is an expanding business.
Our biotechnology stem cells Laboratory offer the whole package of collecting and storing dental stem cells
for a lower cost as compared to cord blood stem cells.
To maintain cell viability, collection kits are prepared to keep cells alive and shelter freshly extracted teeth from temperature changes.
Even with these precautions, the time passed from gathering to arrival at the processing laboratory must be shorter than 72 h
Dental stem cell banking
Dental stem cell banking services .
Dental Stem Cells / Mesenchymal Stem Cells (MSCs) are harvested from the teeth
Stem cell therapy is the new realm of regenerative medicine for Diabetes Type 1, Wound Healing, Parkinson’s, etc.
Stem cell storage.
The approaches used for stem cell storage are:
(a) Cryopreservation (b) magnetic freezing.
Cryopreservation
It is the process of preserving cells or whole tissues by cooling them to sub-zero temperatures.
Cells harvested near end of log phase growth (approximately. 80–90% confluent) are best for cryopreservation.
Liquid nitrogen vapour is used to preserve cells at a temperature of <−150°C.
In a vial 1.5 ml of freezing medium is optimum for 1–2 × 106 cells.
Magnetic freezing
This technology is referred to as cells alive system (CAS), which works on principle of applying
a weak magnetic field to water or cell tissue which will lower the freezing point of that body by up to 6–7°C.
it can increase
the cell survival rate in teeth to 83%.
CAS system is a lot cheaper than cryogenics and more reliable.
All registered participants will receive certificates at the end of the course :
1) “Good Clinical Practice”
2) “Stem Cells therapy Expert”
Interested in learning whether current clinical programs, research developments, or emerging therapeutic approaches may be relevant to your situation?
Educational and research information only. Individual medical decisions should be made in consultation with qualified healthcare professionals.